Oral and Maxillofacial Regeneration
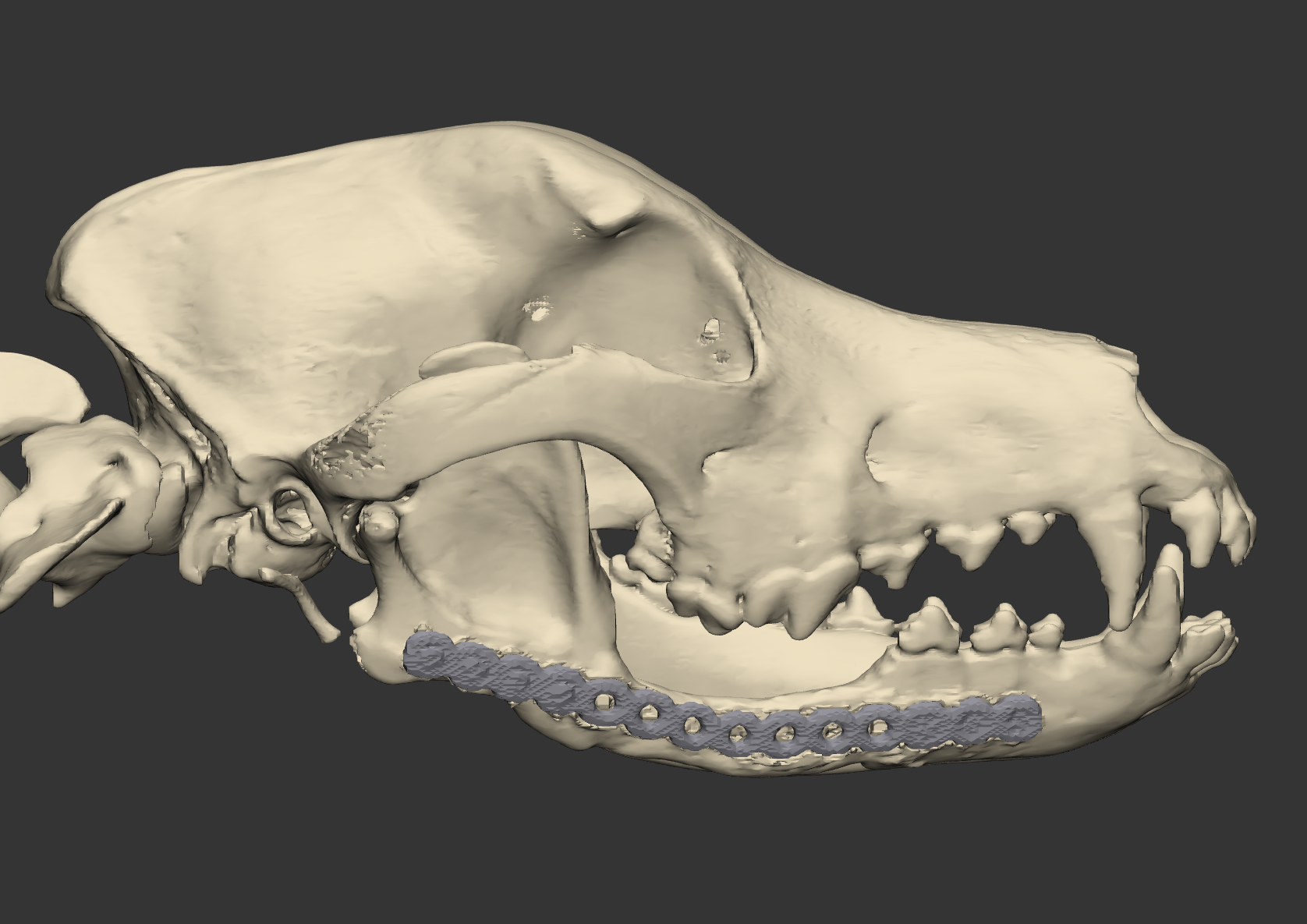
Canine or feline mandibles may need reconstruction due to removal of oral cancerous tissue. The VORL research projects consist of optimum techniques to reconstruct the mandible or temporomandibular joint to allow the animal to return to normal chewing function and facial appearance.
Arthroscopy to the Temporomandibular Joint of Dogs

The temporomandibular joint (TMJ) plays an essential role in the biomechanics of the mammalian jaw, providing essential functions such as chewing, drinking, speaking, and swallowing. TMJ disorders have been identified as significant contributors to orofacial pain and dysfunction in both humans and animals. Among domesticated animals, TMJ disorders in dogs and cats are particularly relevant, with an incidence rate that warrants comprehensive exploration and understanding. The intricacies of TMJ pathology encompass a spectrum of conditions, ranging from degenerative joint diseases, arthritides, to traumatic injuries and neoplasia. In this project, we are establishing precision diagnosis using nanoscope arthroscopy as a valuable tool for both diagnostic and therapeutic purposes in the TMJ of dogs. The adaptation of arthroscopic techniques across species will be contributed significantly to our understanding of TMJ pathology and the development of minimally invasive interventions.



Temporomandibular Joint Replacement
Temporomandibular joint (TMJ) disorders causing structural alteration of the joint typically result in substantial functional deficiencies hindering essential life functions. This project is focusing on the development, validation and clinical implementation of a first-of-its-kind procedure to treat end stage TMJ disorders in dogs and cats. Our group developed a TMJ prosthesis that is specifically adapted to how the jaws and skull are shaped and how they move in relation to each other in cats and in dogs. TMJR in people is now the standard of care. (U.S. Patent Application 63/414,297 filed on October 10, 2022). We are now in a road map for clinical trials and implementations for various TMJ disorders.
Arzi B, Weed ME, Garcia T, Goldschmidt S, Marcellin-Little D. Kinematic performance of a novel temporomandibular joint replacement prosthesis under bite force conditions in dogs and cats . American Journal of Veterinary Research (AJVR), 2024 85(7).



Patent Pending on UC Davis-Designed Temporomandibular Joint (TMJ) Prosthesis for Cats and Dogs
Veterinarians at the UC Davis School of Veterinary Medicine have gained patent pending status on a jaw joint replacement implant for cats and dogs with end-stage temporomandibular joint (TMJ) disorders. The group’s TMJ replacement (TMJR) prosthesis could revolutionize treatment for pets with non-functioning TMJs, either due to injury or disease. Initial research on the TMJR was recently published in the American Journal of Veterinary Research.
Autologous Adipose-Derived Mesenchymal Stem-Cell Therapy for Cats with Chronic, Non-Responsive Gingivostomatitis
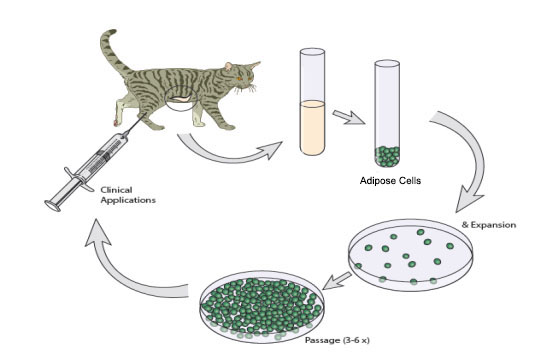
Feline chronic gingivostomatitis (FCGS) is a severe inflammatory oral disease of cats that is often refractory to treatment. The condition is marked by oral inflammation affecting the gingival and non-gingival mucosa, particularly the caudal oral mucosa lateral to the palatoglossal folds. Affected cats typically display clinical signs related to oral discomfort, including inappetence, anorexia and ptyalism. The etiopathogenesis of FCGS is poorly understood. Numerous factors such as breed predisposition, environmental stress, and a variety of infectious agents have been implicated in disease causation; however, the roles of these factors remain unresolved. Current treatment modalities include full or near-full mouth extractions, corticosteroid treatment, antibiotics and pain management. Recently, feline interferon treatment (available in Europe) has been proposed for non-responsive stomatitis. Extraction therapy provides the highest success rate (60%) whereas 40% of the cases will either not respond to extractions or will need additional (often lifelong) medical management.
Reconstruction of critical size mandibular defects using rhBMP2
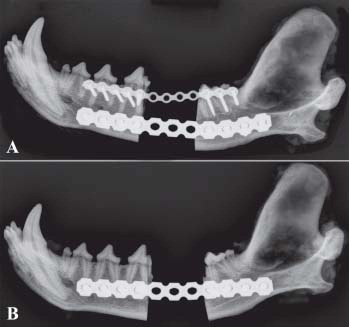
A common result of critical size mandibular bone defects is malocclusion due to mandibular drift. Malocclusion results in difficulty eating and drinking and pain of the contralateral temporomandibular joint (TMJ). The ideal treatment should reconstruct the mandible, potentially through bone regeneration, to restore proper function and pain-free occlusion. In the clinical aspects of this project mandibular reconstruction technique using titanium plates and recombinant human bone morphogenetic protein-2 (rhBMP-2is used. To date, we achieved excellent clinical results with regenerating the mandibular bone in dogs. However, this requires further validation.
First we evaluate the dogs via computerized tomography (CT) as it is a minimally invasive, highly reliable technique that can provide quantitative measures of bone density and porosity, which impact the strength and other mechanical properties of bone. Second, we evaluate the recruitment of circulating mesenchymal stem cells (MSCs) and endothelial progenitor cells (EPCs) as a result of local implantation of a scaffold and rhBMP-2 in the treated dogs.
Temporomandibular joint disorders among the mammalian species
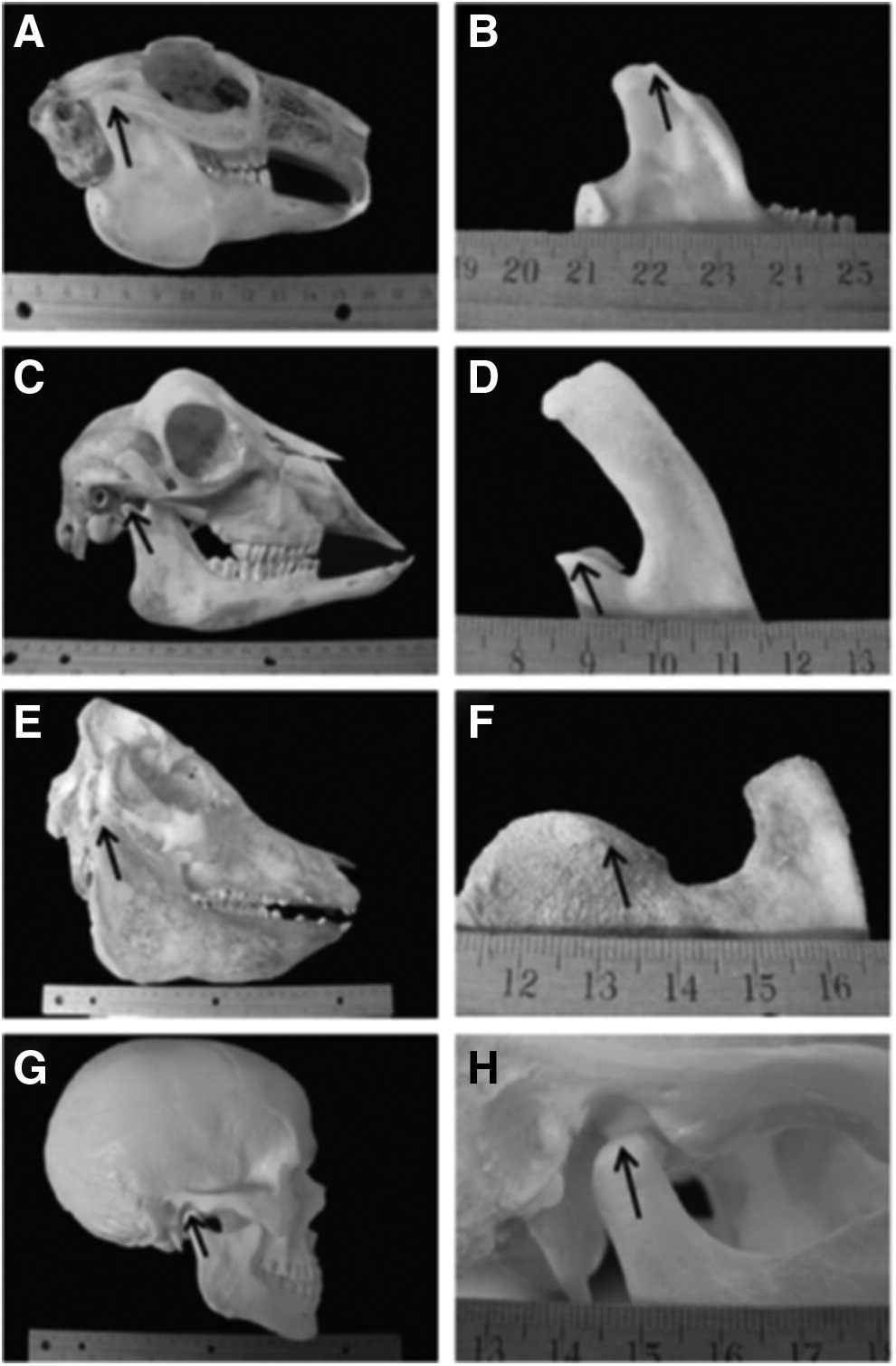
The temporomandibular joint (TMJ) is a feature that is unique to the mammalian species. It is an articulation between the temporal bones and the mandibular head of the condilar process of the mandibles. Between these bones, most mammalians have a fibrocartilagenous disc that separates the joint into two compartments. Each specie has a unique chewing behavior and eating patterns which make this joint somewhat different between the species to accommodate the structure-function relationship.
We study the TMJ disorders occurring among the mammalian species. We utilize our clinical data from the Dentistry and Oral Surgery Service at the VMTH, the radiologic data obtained via computed tomography, pathology specimens and specimens available to us from the California Academy of Science. Combined together, the information allows us a unique insight into TMJ disorders occurring among the mammalian species. The results of our studies are being published in the per-reviewed literature as we progress.
Contacts
Boaz Arzi
Professor
Natalia Vapniarsky-Arzi
Associate Professor
